 In recent years data have been emerging on the association of aortic arch atheromas and cerebral infraction, in particular, when no obvious etiology could be found. Between the heart and the carotid and vertebral arteries there is the aortic arch, an area of difficult access for diagnostic techniques commonly used in daily practice. 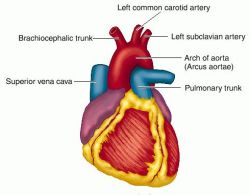
However, in the context of secondary prevention it is essential to reach an etiological diagnosis in order to prescribe the optimal measures for each individual patient, and in this respect, stroke of uncertain etiology remains a great clinical challenge. These secondary prevention strategies include quitting smoking, the administration of aspirin, antihypertensive and lipid-lowering treatments to reduce blood pressure and cholesterol (even when in the "normal" range), surgical or percutaneous interventions on significant stenosis of the symptomatic carotid artery, and anticoagulation in the case of cardioembolism. The management of patients with cerebral infarction focuses on measures that will reduce the risk of stroke recurrence. Despite the use of these diagnostic studies together with routine screening of possible coagulopathy or systemic diseases, and the use of transcranial Doppler sonography with the Valsalva maneuver to rule out the presence of patent foramen ovale with right-to-left shunt, it is not possible to establish a definitive etiologic diagnosis in 10-40% of ischemic stroke patients. Because of the importance of both etiologies, most current protocols for assessing cerebral ischemia include specific radioimaging studies of the cranial arterial system (Doppler ultrasound evaluation of supra-aortic arteries, optionally in association with angiography or magnetic resonance angiography), as well as cardiological studies including electrocardiogram, transthoracic echocardiogram (TTE), and Holter electrocardiographic monitoring if paroxysmal atrial arrhythmias are suspected. Subsequently, it has been shown that approximately 25% of cerebral ischemic events are due to cardioembolism with atrial fibrillation involved in two thirds of these patients, which is a relevant finding to establish a correct diagnosis given the need of anticoagulation and the increasing trend to start anticoagulants very early. Miller Fisher described the trascendental etiological role of artery-artery embolism from carotid atherosclerotic plaques. Basically, this view has changed since 1951, when C. In the first half of the 20th century, it was considered that the majority of cerebral infarctions were due to an episode of vasospasm, but currently this mechanism is not considered of great importance. In addition, another 10% of deaths are related to the consequences and complications following cerebral infarction. With the progressive increase in life expectancy in Western populations, the incidence of cerebral ischemic diseases has become a direct cause of death of 10% of the general population. However, given the limited data available and its retrospective nature, randomized prospective studies are needed to establish the optimal secondary prevention therapeutic regimens in these high risk patients. In a retrospective case-control study, statins significantly reduced the relative risk of new vascular events. In non-randomized retrospective studies anticoagulation was superior to antiplatelet therapy in patients with stroke and aortic arch plaques with mobile components. In addition, the impact of complex plaques (≥ 4 mm thick, or with mobile components) on increasing the risk of stroke is also reviewed. 
Here we review the evidence of aortic arch atheroma as an independent risk factor for stroke and arterial embolism, including clinical and pathological data on atherosclerosis of the thoracic aorta as an embolic source. In these cases, aspirin might not prevent adequately new arterial ischemic events especially stroke. The association with ischemic stroke was particularly strong when atheromas were located proximal to the ostium of the left subclavian artery, when the plaque was ≥ 4 mm thick and particularly when mobile components are present. Several autopsy series and retrospective studies of cases and controls have shown an association between aortic arch atheroma and arterial embolism, which was later confirmed by prospectively designed studies. However, in the last two decades, the use of transesophageal echocardiography in patients with stroke of uncertain etiology reveals atherosclerotic plaques in the aortic arch, which often protrude into the lumen and have mobile components in a high percentage of cases. In many stroke patients it is not possible to establish the etiology of stroke. 
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
